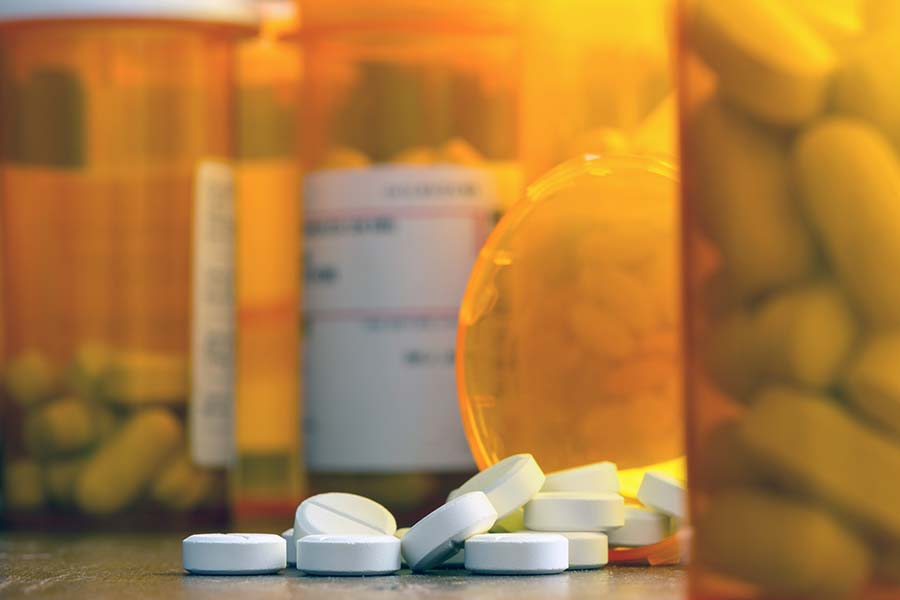
The ongoing opioid overdose crisis has prompted the CDC to take action in the form of developing new guidelines for qualified prescribers.
First and foremost, the CDC stresses that opioid therapy should be utilized only if all other treatment options have been exhausted. Opioids can vastly improve functionality and quality of life, but the benefits must be weighed against the risks of tolerance, addiction, overdose, etc. If opioids are absolutely necessary, the prescribing physician and patient should work together to formulate a safe plan of approach and establish realistic treatment goals before starting therapy. These goals should be re-assessed throughout the course of treatment to ensure that the patient is still experiencing significant improvement.
What does the CDC recommend for pain treatment therapy?
The CDC recommends that patients start off their therapy by taking low doses of short-acting opioids. The use of high dosage and/or extended-release (long acting) opioids is risky and warned against unless the alternatives are ineffective. Additional precautions should be taken when increasing dosage to 50mg or more per day in morphine equivalents, and increasing dosage by 90 mg or more per day is strongly discouraged. Patients with acute pain should be given a minimal amount of pills initially, as studies have shown that a three-day supply is usually sufficient for non-traumatic instances. This policy would lower the likelihood of abuse and protect short-term users from addiction.
One of the most important factors of safe opioid use is continuing patient-physician communication. Providers should schedule a follow-up appointment within one to four weeks of starting a patient on long-term opioid therapy and/or increasing the prescribed dose. Additional appointments should be scheduled at least once every three months, and the risks and benefits of continued opioid use should be considered on a regular basis. Risk management strategies should continually be revisited and naloxone should be made available to patients in order to decrease the chance of opioid-related harm.
What should physicians do?
Physicians should keep track of patient medication records and addictive tendencies to determine risk of overdose. High-risk patients should be instructed to take additional precautions and avoid drug combinations that could prove lethal. For example, patients taking benzodiazepines should avoid taking opioids concurrently whenever possible. Physicians should also monitor patient drug use through regular urine drug screens. If evidence arises that a patient is suffering from opioid use disorder, the provider should arrange for enrollment in an evidence-based treatment plan. These typically involve opioid-agonist therapy along with behavioral and talk therapy.
How have patients responded to these guidelines?
Patients with chronic pain have responded to these guidelines with disdain, arguing that the CDC is imposing restrictions unreasonably. The FDA is typically responsible for ensuring safe drug prescription, but the CDC is stepping in to regulate the spread of opioids anyway, claiming that these guidelines were reviewed by experts and will significantly reduce overdose deaths. Activists in the pain community argue that these rules are hardly going to affect death rates and will only make life harder for legitimately suffering chronic pain patients.
While the CDC’s plan may be well intentioned, it is an insufficient and misguided attempt to affect change without improving patient care. A majority of opioid users become abusers because of inadequate treatment, not because of loose controls; for example, many turn to the streets for drugs when they are not being prescribed the correct medicines or dosages to manage their pain. The CDC guidelines are focused on regulations and restrictions instead of quality of care, a decision that is only going to exacerbate the opioid overdose problem.
Pain treatment is a holistic process, and an ideal recovery scenario includes physical therapy, occupational therapy, therapeutic recreation, psychological services, pain education, relaxation training, vocational rehabilitation, and finally medical management. Instead of limiting the options that are available to patients, the CDC should be raising awareness about the various treatment possibilities that exist. Perhaps the country will see a decrease in opioid abuse once patients have access to the care they desperately need.
Alternative Care Plans for Chronic Pain
(A Selection of Methods to Try Before Seeking Opioids)
Physical therapy utilizes treatment strategies designed with your personal needs in mind. A trained physical therapist will conduct a comprehensive assessment prior to initiation in order to assess your capacity for movement. They will ask you about your treatment goals and help you set forth a realistic plan for the future. Regular sessions can reduce the pain and soreness caused by everyday activity, and can help you to avoid, or at least delay, surgery or prescription drug use.
Occupational therapy is a means of enabling participation in normal, everyday activities. A trained occupation therapist will conduct a comprehensive assessment prior to initiation in order to assess your strengths, weaknesses, and lifestyle choices. Through regularly scheduled sessions and practice, you can devise methods of relieving the discomfort caused by various activities.
Therapeutic recreation, otherwise known as recreational therapy, uses active involvement in leisure activities to address the psychological and physical needs of participants. One of the main ideas behind this sort of treatment is that active participation in leisure activities greatly improves quality of life. Individuals with chronic pain often report missing out on experiences due to restrictions; recreational therapists work to make sure this happens as infrequently as possible. Examples of therapeutic interventions include: water therapy, horseback riding, music programs, outdoor adventures, creative arts, animal assisted therapy, etc.
Psychological services are just as important as physical health services for individuals with chronic pain. Emotional distress plays a large role in the perceived intensity of pain, so processing and management sessions with a trained professional are highly recommended. Mental health professionals can teach you coping skills, help you to gain insight into your pain and triggers, recommend lifestyle changes, and so much more.
Pain education is important for both the chronic pain survivor and their friends and family. The concept of continuous pain can be hard to understand for those who are not experiencing it; sharing facts and literature on the subject can help others to respond more appropriately to your situation. Physicians and patients alike should be educated on the proper utilization of opioids in order to avoid unnecessary treatment and/or addiction in the future.
Relaxation training can be a great coping mechanism for chronic pain. Active relaxation increases blood flow throughout the body and promotes loose muscles and joints. Relaxation can be used to manage ongoing pain symptoms or be used as a means of pain prevention.
Vocational rehabilitation services are designed to offer career opportunities for individuals with physical disabilities. This option is great for people with chronic pain who want to find manageable employment and socialize with others in the workforce. Having a job that is practical for your level of chronic pain can reduce the frequency of flare-ups, relieve stress, and generally make life more enjoyable.
Source Cited: http://www.painnewsnetwork.org/stories/2015/9/16/cdc-opioids-not-preferred-treatment-for-chronic-pain